Quality Insights
Improve value-based care quality and population health outcomes
The rise of value-based care has inevitably spurred heightened focus on quality improvement across the healthcare ecosystem. There are two sides to this coin: measures and members. On the measures side, health plans are working to align with strict national standards and state-specific requirements (think: HEDIS, Star ratings). On the members side, payers are striving to understand their patient populations more fully and provide more timely, appropriate interventions.
Delivering comprehensive solutions to enhance performance and outcomes
Challenge
Solution
Siloed, incompatible information from EMRs, claims and other sources hinder efficient quality calculations and data submission
Challenge
Solution
Unnecessary ED visits and readmissions drive up costs and decrease member satisfaction
Challenge
Solution
Insufficient, unreliable data on clinical performance deters provider engagement
Celebrating big wins with Quality Insights
Analytics in action
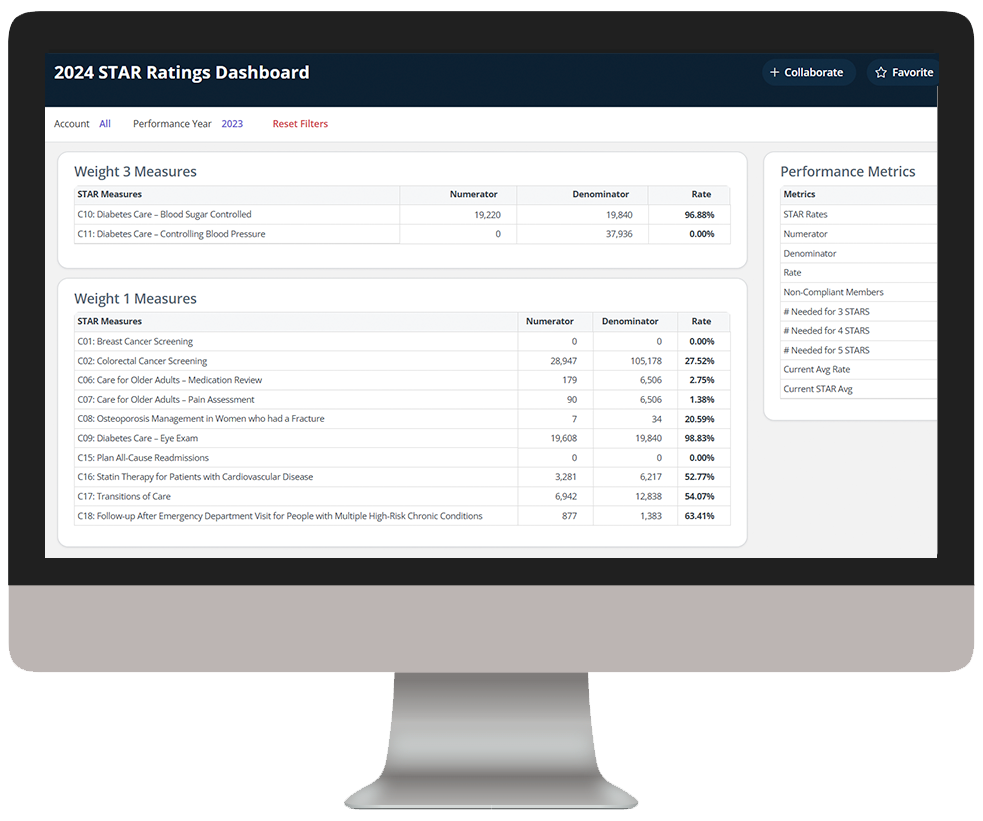
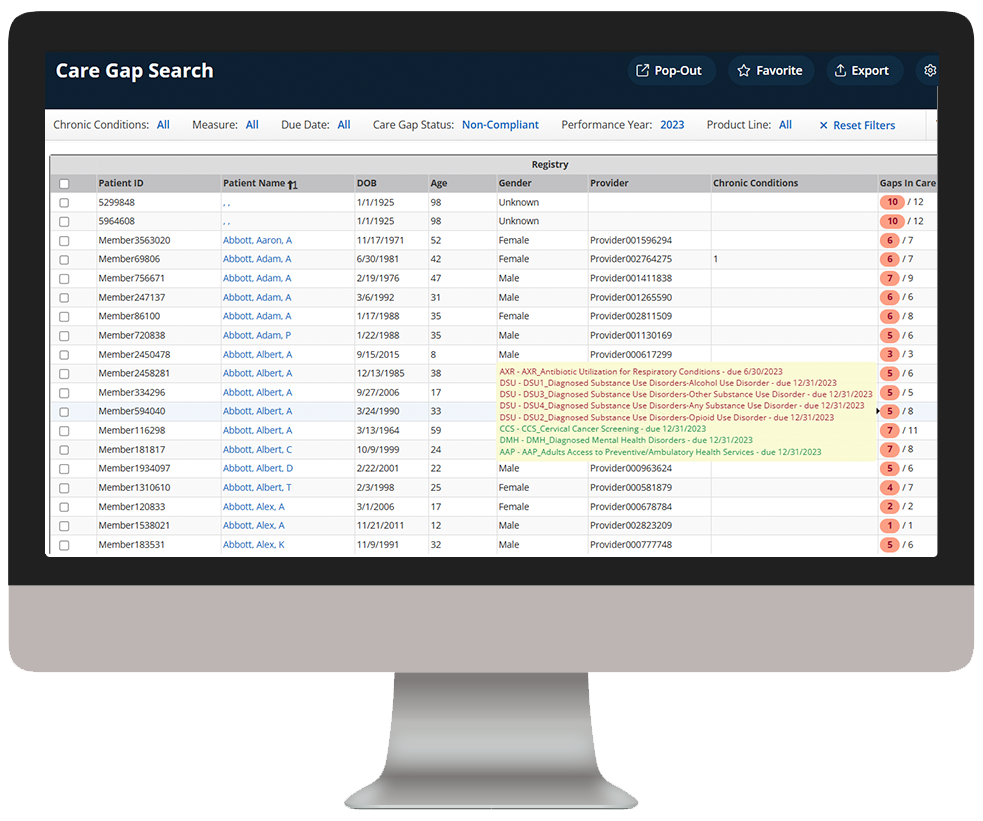
Our intelligent platform and intuitive user interface make it easy to unlock the value of your data. In as little as three clicks, we bring meaningful insights, powerful visualization, and analytics innovation to help you make an even bigger impact at your organization.
As you click through our example dashboards, hover over the image to explore a few key features.
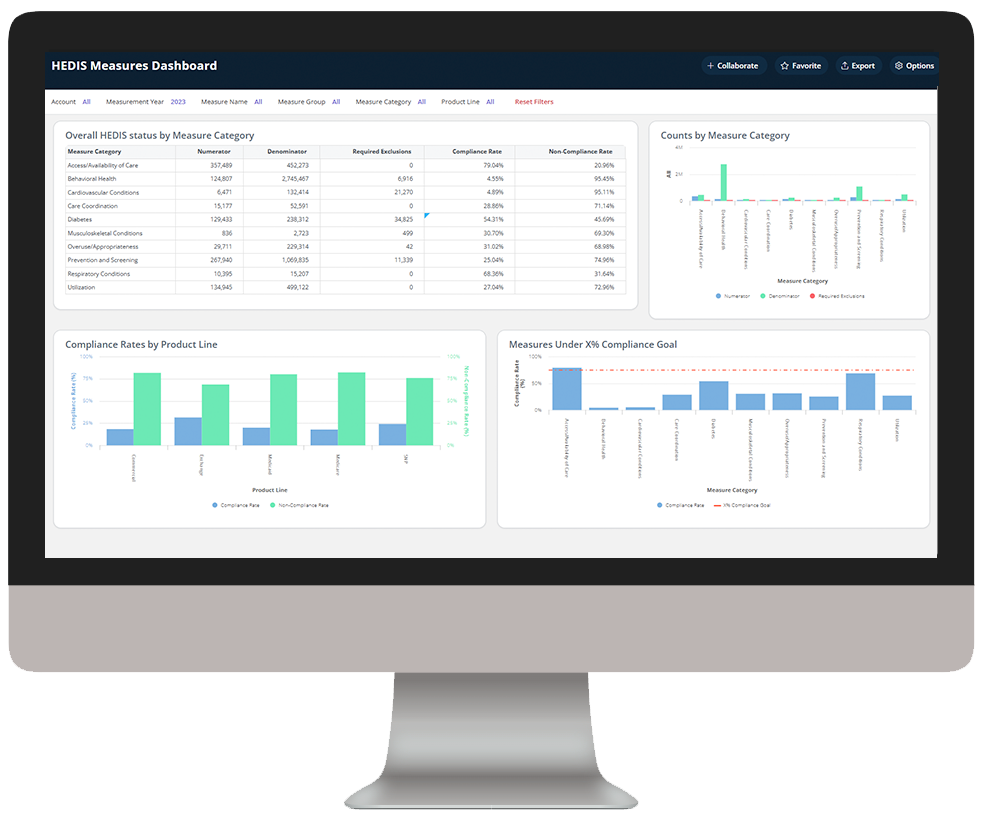
Assess HEDIS measure performance and compliance
Dive deeper into Quality Insights
Download the data sheet to see how Quality Insights can help your health plan improve care quality and outcomes.
Visit our Value-Based Care Blueprint page for everything you need to know to navigate the intersection of value and analytics.
Get our take on industry trends
2022 Rx: Your new, post-pandemic prescription for success
By Dave Schweppe, Chief Analytics Officer, MedeAnalytics Despite the common use of the term “post-COVID,” most leaders across the healthcare…
Read on...Combating the opioid epidemic in North America with Nobel Prize winning research
American Researchers Dr. David Julius and Dr. Ardem Patapoutian from California were awarded the Nobel Prize in medicine for their path breaking work on the development of non-opioid painkillers, showing immense promise for combating the epidemic.
Read on...Why managed Medicaid/Medicare health plans need analytics to improve outcomes
Managed care organizations that provide healthcare services to Medicare/Medicaid members are dedicated to improving the health and wellness of these underserved populations, especially those living in rural areas.
Read on...Using consumer analytics to steer health-related decisions
Companies tap into what people like to eat and drink, how we purchase consumables, where we like to shop, what shows we might like to stream, whether we vote, and so on. If you have ever created a profile on a streaming application (think Netflix or Amazon), you will receive recommended books, movies and other items just as soon as you start surfing.
Read on...Want to talk with one of our experts?
Payer Value Analytics: Our full lineup of payer solutions
Everything you need to step into the future of healthcare and drive real change across populations.

Quality Insights
Activate insights into population health and quality to improve satisfaction and outcomes for members and maintain a competitive position in the market.

Employer Insights
Elevate data sharing with employer groups to demonstrate plan value and increase efficacy of risk stratification and care management plans.

Network Insights
Accelerate provider performance with evidence-based outcomes comparisons, cost-effectiveness analyses, and extensive segmentation capabilities.