Employer Insights
Focused, real-time analytics cultivates loyalty and retention of commercial clients
As membership steadily declines, health plans are experiencing intensified pressure to demonstrate effectiveness and value to commercial accounts. Data-powered, actionable insights are mission-critical to improving efficiency and responsiveness, augmenting transparency in reporting, and empowering employers and brokers with the information they need to manage costs effectively.
Delivering comprehensive solutions to your employer relationship challenges
Challenge
Solution
Lack the analysis and automation capabilities employers require to fully understand and support their populations
Challenge
Solution
Insufficient, inconsistent services result in disengaged, dissatisfied employers and brokers
Challenge
Solution
Struggle to prove value and worth of health plan to commercial accounts
Celebrating big wins with Employer Insights
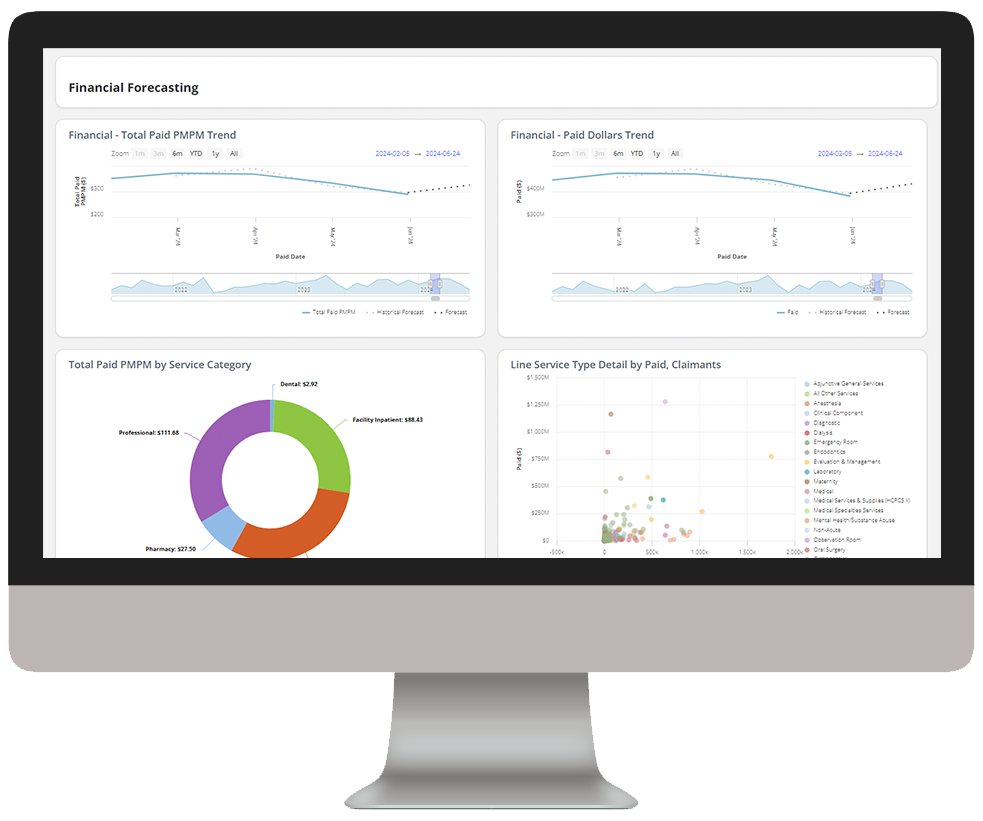
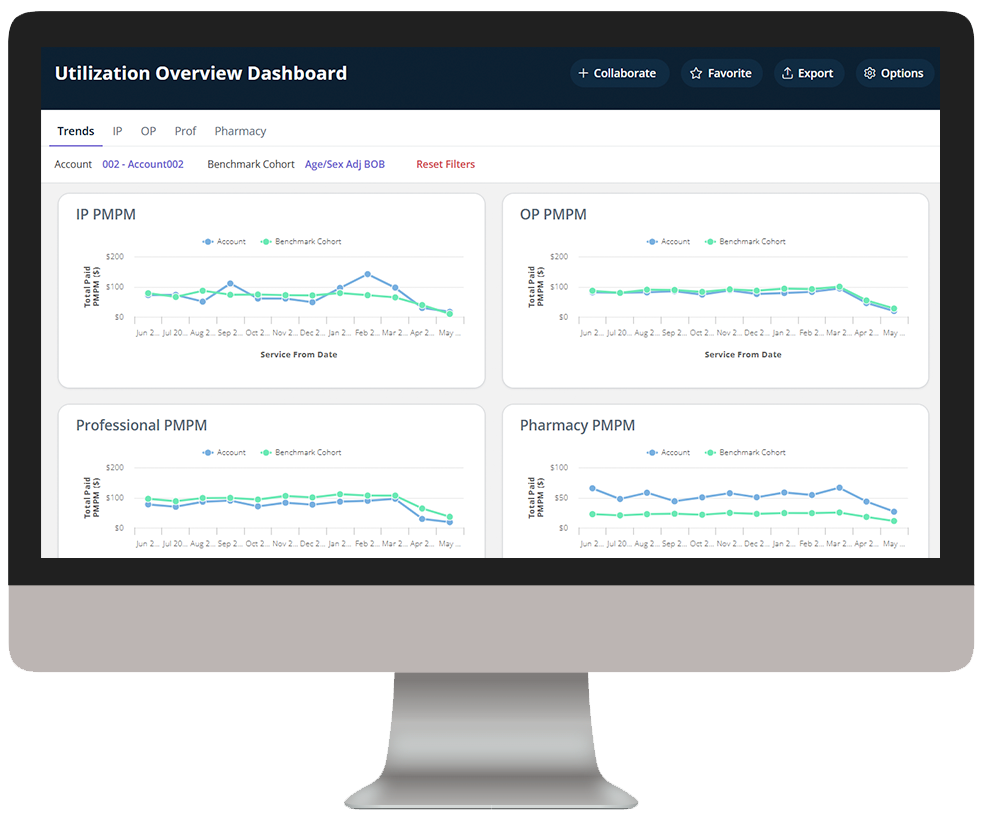
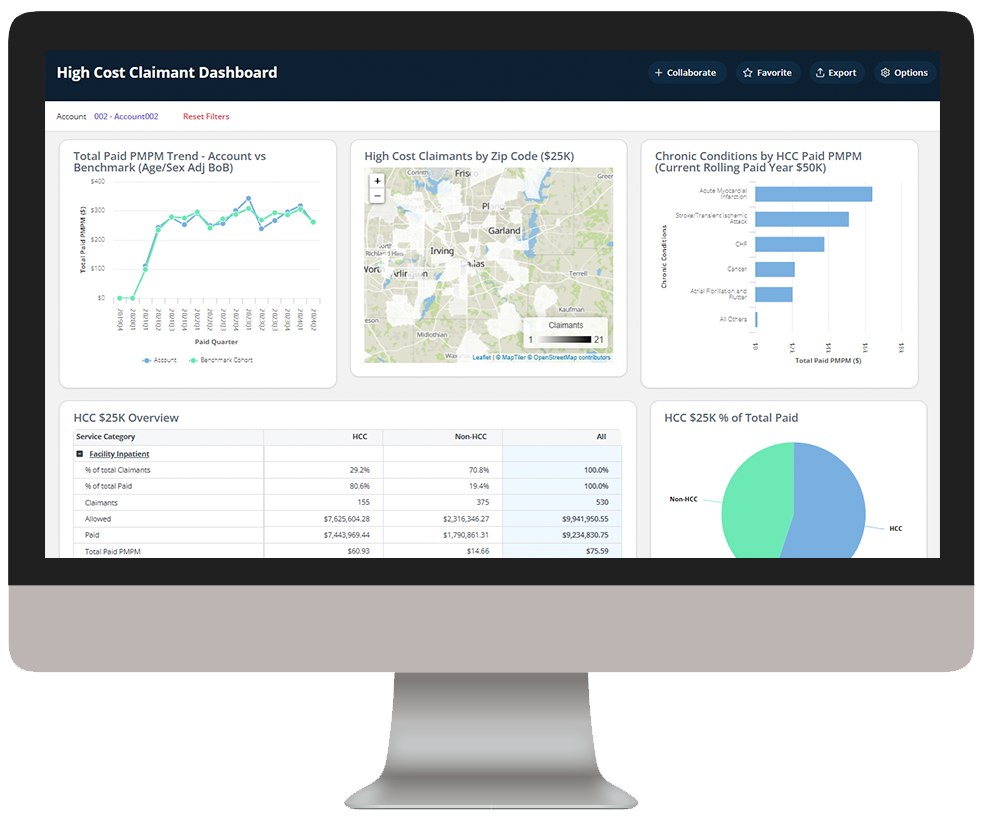
Analytics in action
Our intelligent platform and intuitive user interface make it easy to unlock the value of your data. In as little as three clicks, we bring meaningful insights, powerful visualization, and analytics innovation to help you make an even bigger impact at your organization.
As you click through our example dashboards, hover over the image to explore a few key features.
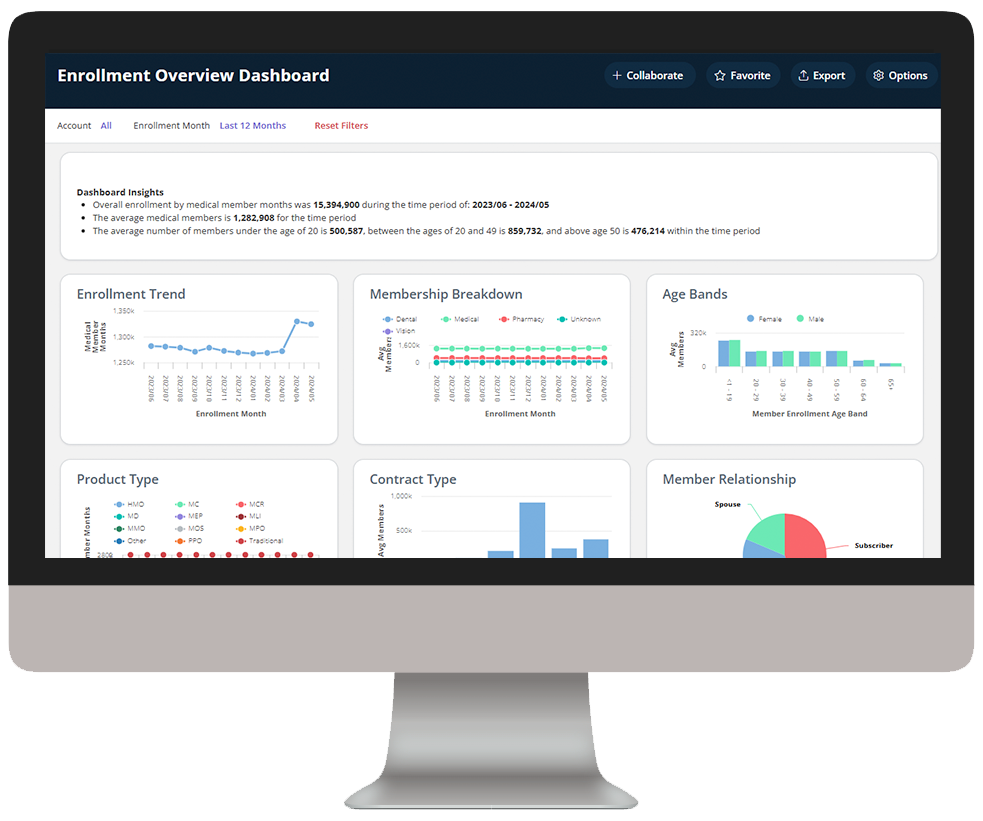
Assess enrollment trends and metrics to inform plan design decisions
Dive deeper into Employer Insights
Download the data sheet to learn more about how Employer Insights can help you remain competitive in an aggressive market.
Download the data sheet to learn more about how Stop Loss can help you monitor and manage the financial impacts of high-cost claimants.
Want to talk with one of our experts?
Payer Value Analytics: Our full lineup of payer solutions
Everything you need to step into the future of healthcare and drive real change across populations.
Quality Insights
Activate insights into population health and quality to improve satisfaction and outcomes for members and maintain a competitive position in the market.
Employer Insights
Elevate data sharing with employer groups to demonstrate plan value and increase efficacy of risk stratification and care management plans.
Network Insights
Accelerate provider performance with evidence-based outcomes comparisons, cost-effectiveness analyses, and extensive segmentation capabilities.
Get our take on industry trends
AHIP26: Turning Healthcare Complexity into Measurable Performance
Health plans are navigating rising medical costs, intensifying regulatory demands, margin pressure, evolving member expectations, and growing operational complexity, all…
Read on...The Medicare Advantage retention gap: Turning member experience into a growth strategy
Growth in Medicare Advantage has become increasingly difficult to sustain. Acquisition costs are rising, competition is intensifying, and members are…
Read on...Why “good” isn’t good enough: The hidden cost of sub-4 Star Medicare Advantage performance
Healthcare outcomes have never mattered more, and achieving exceptional performance has never been harder. Many mid-to-large health plans are below the 4-Star threshold in Medicare Advantage (MA).…
Read on...From conversation to coordination: Key takeaways from OpsIgnite 2026
OpsIgnite 2026 brought together operational leaders from across the Blues ecosystem for four days of candid conversation, practical insights, and…
Read on...