Medicaid Enterprise Analytics
Improving health management for your most at-risk members
With razor-thin margins on reimbursements and more value-based care at-risk contracts, health plans are clamoring for new and innovative ways to address the health of growing Medicaid populations. By mining insights from claim and clinical data, MedeAnalytics provides the foundation for managed care plans and agencies to collaborate and help deliver better outcomes to underserved populations.
Applying data to create person-centered care
Challenge
Solution
Lack of insight into actual impact of social determinants of health within membership limits efficacy of value-based care
Challenge
Solution
Disjointed data sources hinder understanding of member utilization trends and program outcomes
Challenge
Solution
Basic, low-detail view of member health statuses and population patterns stunts plan expansion
Analytics in action
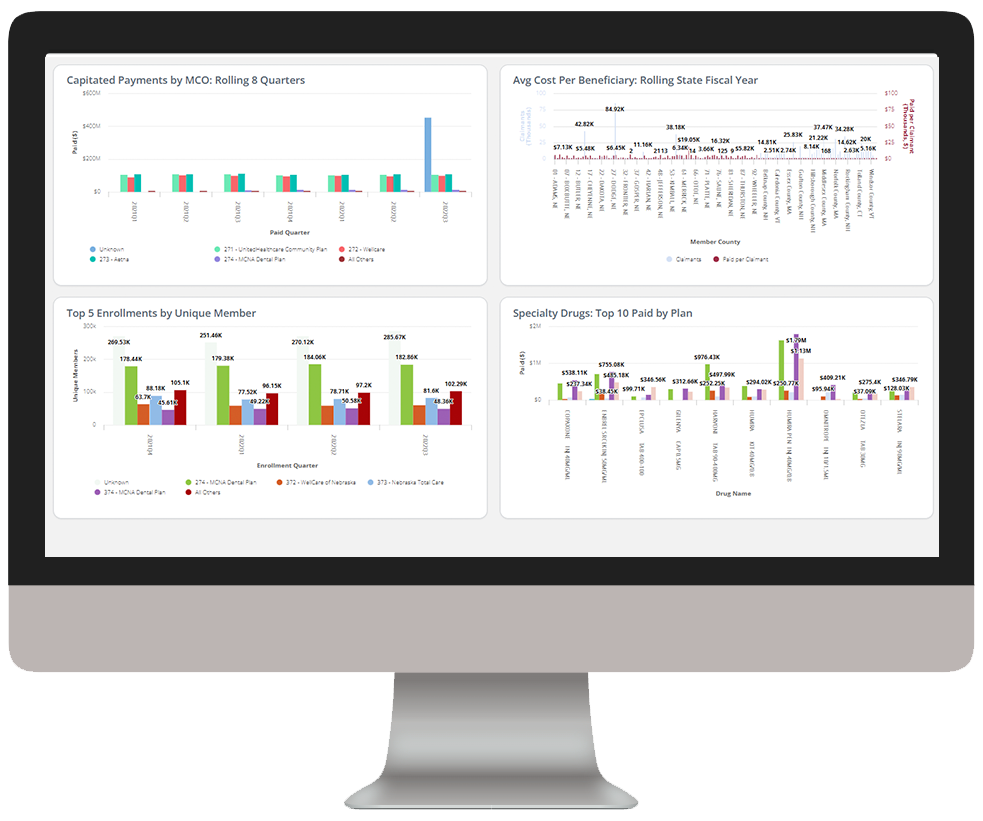
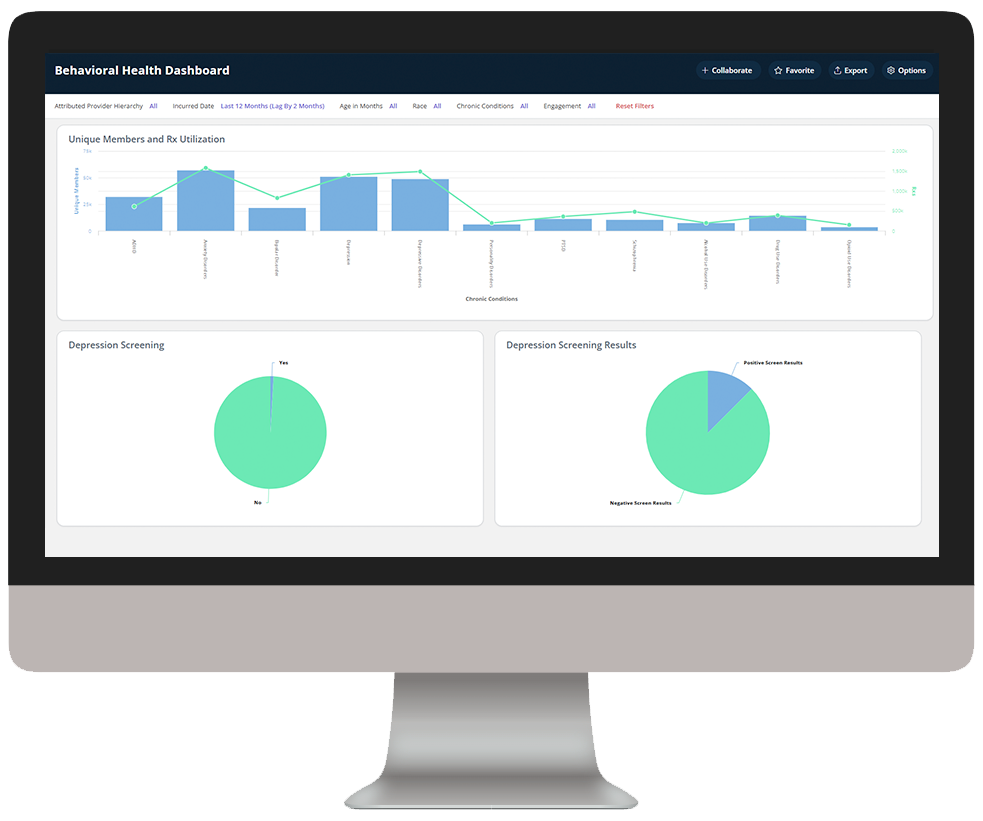
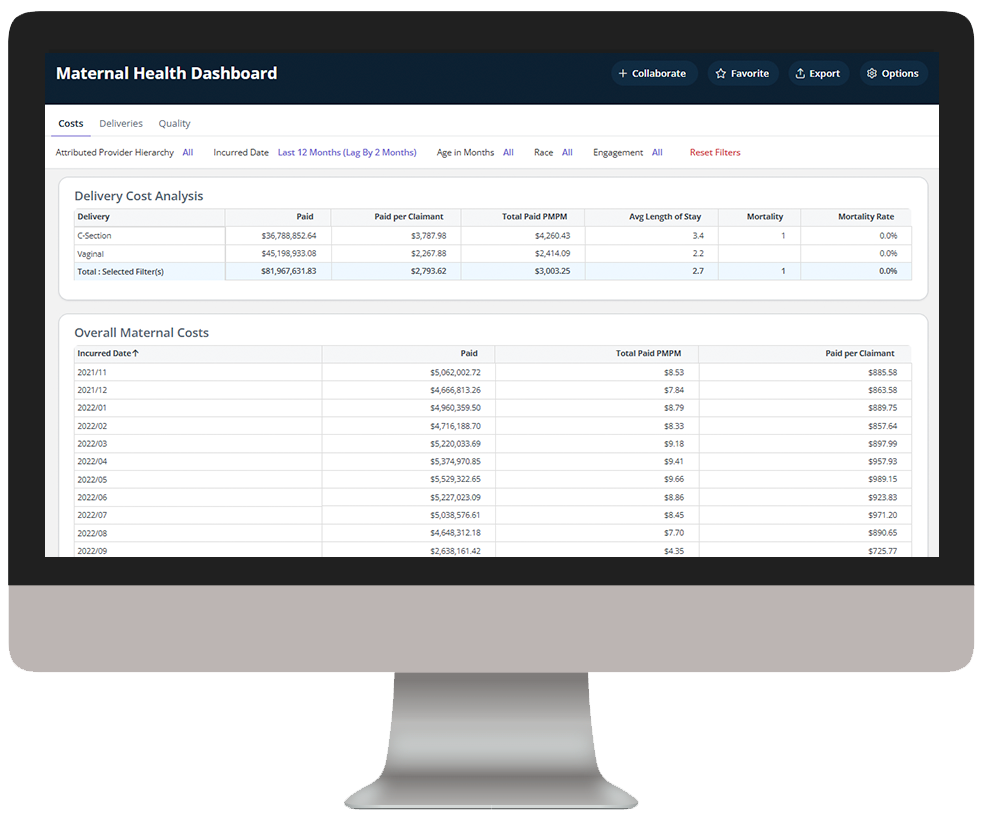
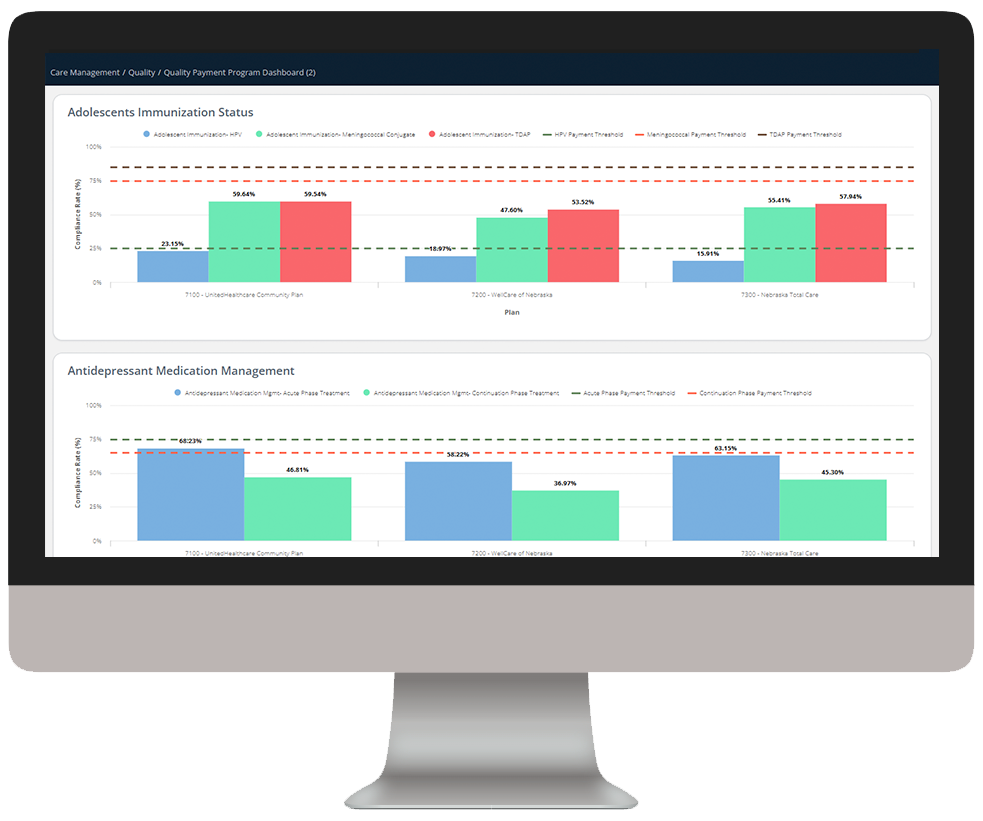
Medicaid Enterprise Analytics delivers key insights into Medicaid beneficiary data, enabling health plans to understand cost drivers, gaps in care, and demographic and SDOH impact to improve care outcomes.
Explore a few key features by hovering over the images below.
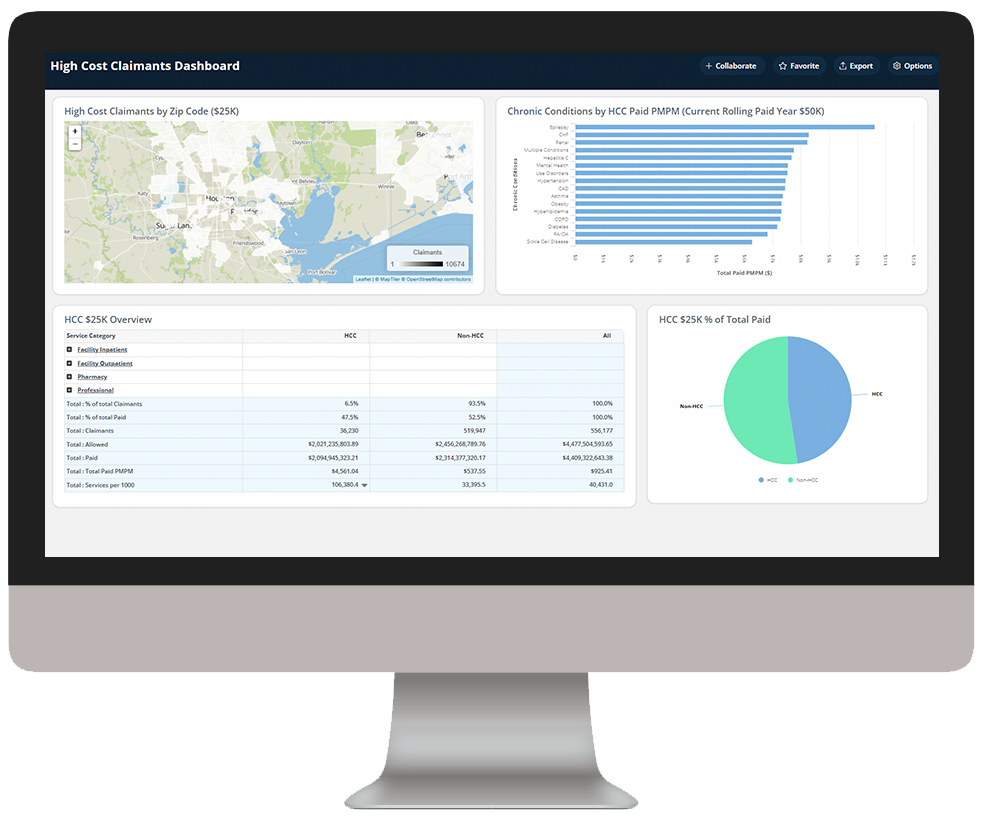
Identify high-cost claimants to prioritize for care management
Dive deeper into Medicaid Enterprise Analytics
Download the data sheet to see how Medicaid Enterprise Analytics integrates traditionally disparate data sources to provide the visibility and transparency health plans need to holistically manage member care.
Get our take on industry trends
The Real Payback of Healthcare Analytics: Key Questions from Healthcare Leaders Around the Nation
MedeAnalytics hosted a Fierce Healthcare webinar featuring key senior leaders from three preeminent healthcare organizations in the U.S: At the…
Read on...The future of digital health part 4: Convergence of AI and analytics for healthcare payers
This post is the fourth and final of our Digital Health series, featuring healthcare visionary and thought leader Andy Dé. In this series, Dé has been discussing how COVID-19 has triggered remarkable digital transformation and uncovers five long-term innovation implications that providers, healthcare leaders, and payers need to consider.
Read on...Use SDOH + Analytics to power better outcomes for underserved population
Whether you’re a payer, provider or patient, on the front lines of care, sitting in front of a computer or receiving treatment, you’ve been affected by the pandemic. Of all the groups who participate in healthcare in one way or another, perhaps no single group has suffered more over the last year during the pandemic than the underserved— those people without ready access to needed healthcare services.
Read on...Go beyond recognition: Use data to take meaningful action this Nurses Week
Since 1994, America has observed National Nurses Week annually from May 6-12. This year more than ever before, it’s critical that healthcare organizations go beyond recognition and start taking action to more effectively support and serve nurses.
Read on...Want to talk with one of our experts?
We're driving data-powered improvement across the industry

Healthcare providers and health systems
Healthcare Providers and Health Systems
use our end-to-end revenue cycle management analytics to lower denials, accelerate A/R, and improve staff productivity.

Healthcare payers and health plans
Healthcare Payers and health plans
deploy our value-based care and provider network analytics to enhance population health, quality and network management and empower their employers and brokers through self-service analytics.

Government Medicare and Medicaid programs
Government Medicare and Medicaid programs
Government Medicare and Medicaid programs rely on our comprehensive dashboards to understand cost drivers, gaps in care, and social determinants impacting beneficiary outcomes.