Workforce Performance Insights
Connecting data to cultivate financial health
Provider organizations house large quantities of data on front-end patient interactions. When applied correctly, that information can be leveraged to understand payment outcomes, correlate encouraged actions to financial gains, and identify training opportunities for revenue cycle management teams. Unfortunately, most information systems are not equipped to execute this type of analysis. With MedeAnalytics Workforce Performance Insights, we are connecting critical registrar and patient access information with back-office financial data to improve team efficiency and cultivate financial health.
Part of the Workforce Quality Insights suite:
Aligning registrar performance to patient experience goals
Challenge
Solution
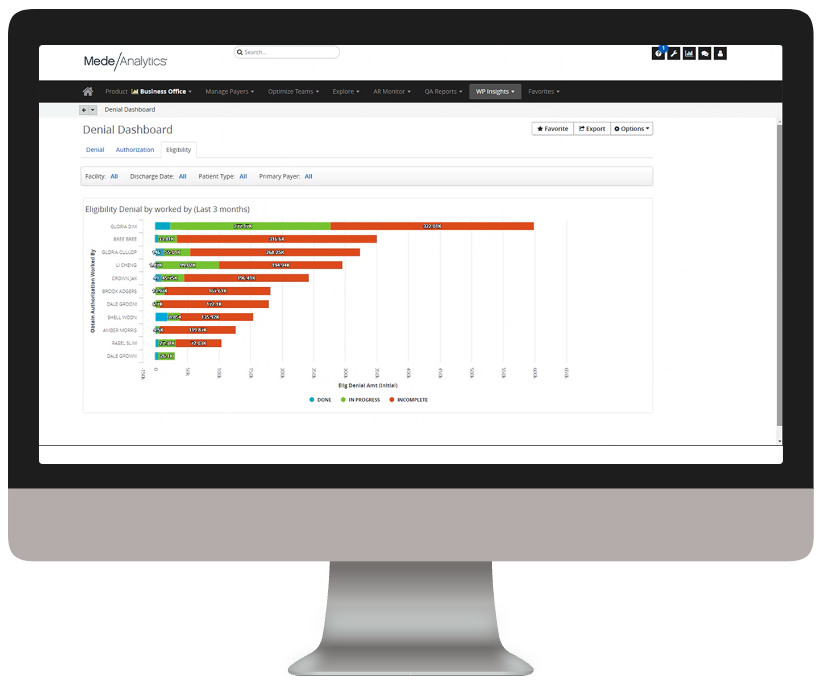
Incorrect estimates for non-emergent care lead to outstanding accounts receivable and time-consuming follow up
Challenge
Solution
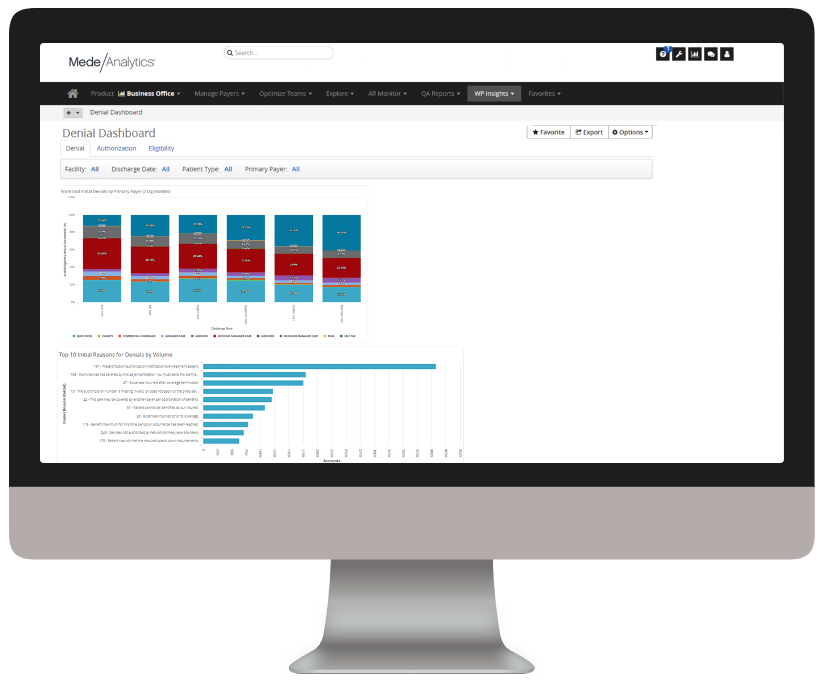
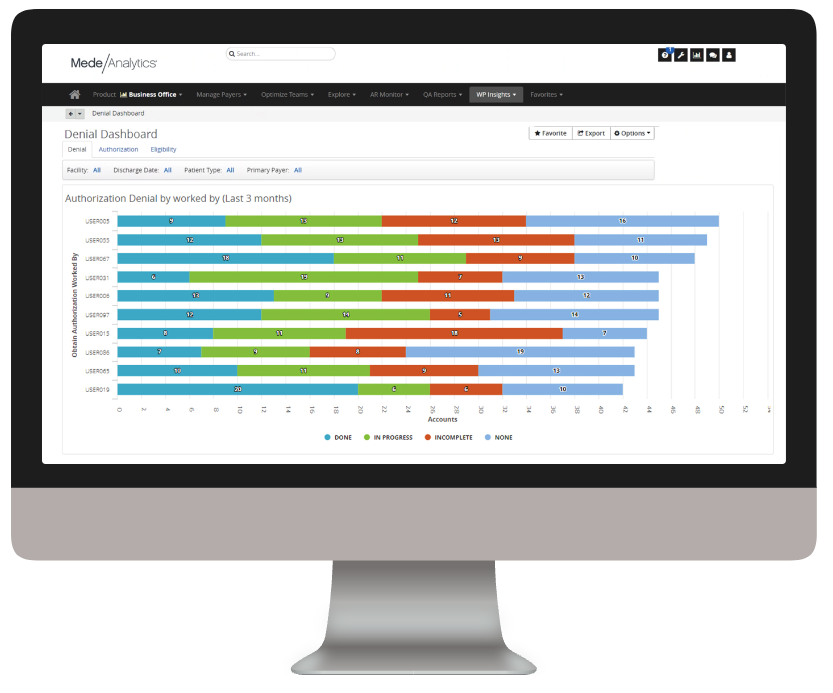
Lack of specificity in denials reporting results in repeated mistakes and decrease in trust
Analytics in action
Our intelligent platform and intuitive user interface make it easy to unlock the value of your data. In as little as three clicks, we bring meaningful insights, powerful visualization, and analytics innovation to help you make an even bigger impact at your organization.
Explore a few key features by hovering over the image.
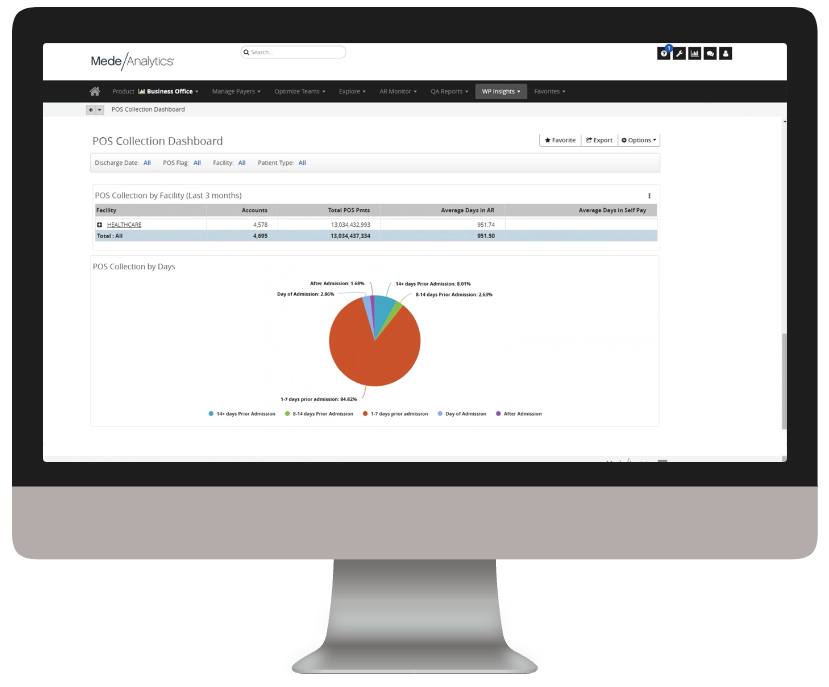
Quickly toggle between dashboards on Collections, Denials, Estimate Accuracy and personalized reports
See when and where you are having success with POS collections to create best practices and determine where you can make improvements
Export results to others or for use in presentations to quickly show how pre-service activities are affecting financial results
Dive deeper into Workforce Performance Insights
Download the data sheet to see how Workforce Performance Insights helps you connect workflow activities and financial outcomes to protect patient financial experience and ensure organizational stability.
Get our take on industry trends
Data visualization: A picture is worth a thousand…healthcare data points?
The amount of data produced daily has grown exponentially with nearly 90% of the world’s data generated in the last two years alone. To ensure we can make sense of this data, analysts must find meaningful ways to present the information to their audiences.
Read on...How did we get here? Hospital analytics and the new normal
I have heard the word “unprecedented” so many times in 2020 that it has lost its significance; many of us have become desensitized to the extraordinary changes in the world this year.
Read on...Avoid COVID-19 modeling pitfalls by eliminating bias, using good data
COVID-19 models are being used every day to predict the course and short- and long-term impacts of the pandemic. And we’ll be using these COVID-19 models for months to come.
Read on...Population Health Amid the Coronavirus Outbreak
In speaking with many colleagues throughout the provider and payer healthcare community, I’ve found an overwhelming sense of helplessness to the outbreak’s onslaught. This is exacerbated by the constant evolution of reported underlying medical conditions that indicate a higher risk of hospitalization or mortality for a coronavirus patient.
Read on...Want to talk with one of our experts?
Provider Value Analytics: Our full lineup of provider solutions
Everything you need to support your front office, mid-cycle and back office.

Patient
Access
Insights
Optimize patient satisfaction during the patient registration and payment clearance processes with critical, real-time analytics information.

Revenue Integrity
Suite
See how clinical operations affect your bottom line with complete visibility into compliance risk and clinical documentation performance.

Business Office
Suite
Achieve optimized cash flow and operational excellence with big-picture insight into opportunities for improving collection rate, denials, and staff productivity.

Workforce Quality Insights
Use powerful analytics capabilities to generate end-to-end insights into how patient access activities are impacting the back-office outcomes.
See the solution ❯

Cost
Insights
Drill down into claims and encounter-level data to target and align controllable costs with outcomes and reimbursement.