Employer Group Performance
Deliver the transparency, intelligence, and interactive experience that will thrill your employer groups
Why traditional employer reporting falls short in a more demanding market.
Employer groups and brokers expect transparent, interactive, and actionable insights that help them understand plan performance, manage costs, improve outcomes, and make more confident benefit decisions.
Many health plans rely on fragmented reporting processes, disconnected data sources, and manual workflows that make it difficult to deliver timely, decision-ready insights. Without a unified view across cost, utilization, risk, benchmarks, and social determinants of health, plans struggle to demonstrate value, support renewals, and differentiate in a competitive market.
“As we moved into this self-service analytics environment with Employer Insights, we noticed a meaningful increase in customer satisfaction. The ability to provide our brokers and employers with real-time data and analytics insights has been critical to our success. Since deployment, we won back many of the contracts that we’d lost in prior years – including some of the largest clients within the state – and gained a significant list of new customers as well.”
Manager, Employer Analytics, Northeast Health Plan
MedeAnalytics offers a smarter approach to employer group performance.
Move from static reports to interactive, employer healthcare analytics.
MedeAnalytics delivers a real-time, interactive reporting experience with AI-powered insights that empower employer groups and brokers to drive action and decision-making while reducing internal burden and strengthening relationships.
With MedeAnalytics, you can:
- Provide a complete, integrated view of plan performance
- Enable self-service analytics for employers and brokers
- Support renewals with compelling, data-driven storytelling
- Benchmark performance against your book of business
- Improve plan design using predictive insights
- Increase reporting speed and accuracy

MedeAnalytics Employer Group Performance is built to deliver measurable and meaningful, decision-ready insights and action by combining AI-powered analytics, advanced data integration, and intuitive, transparent reporting.
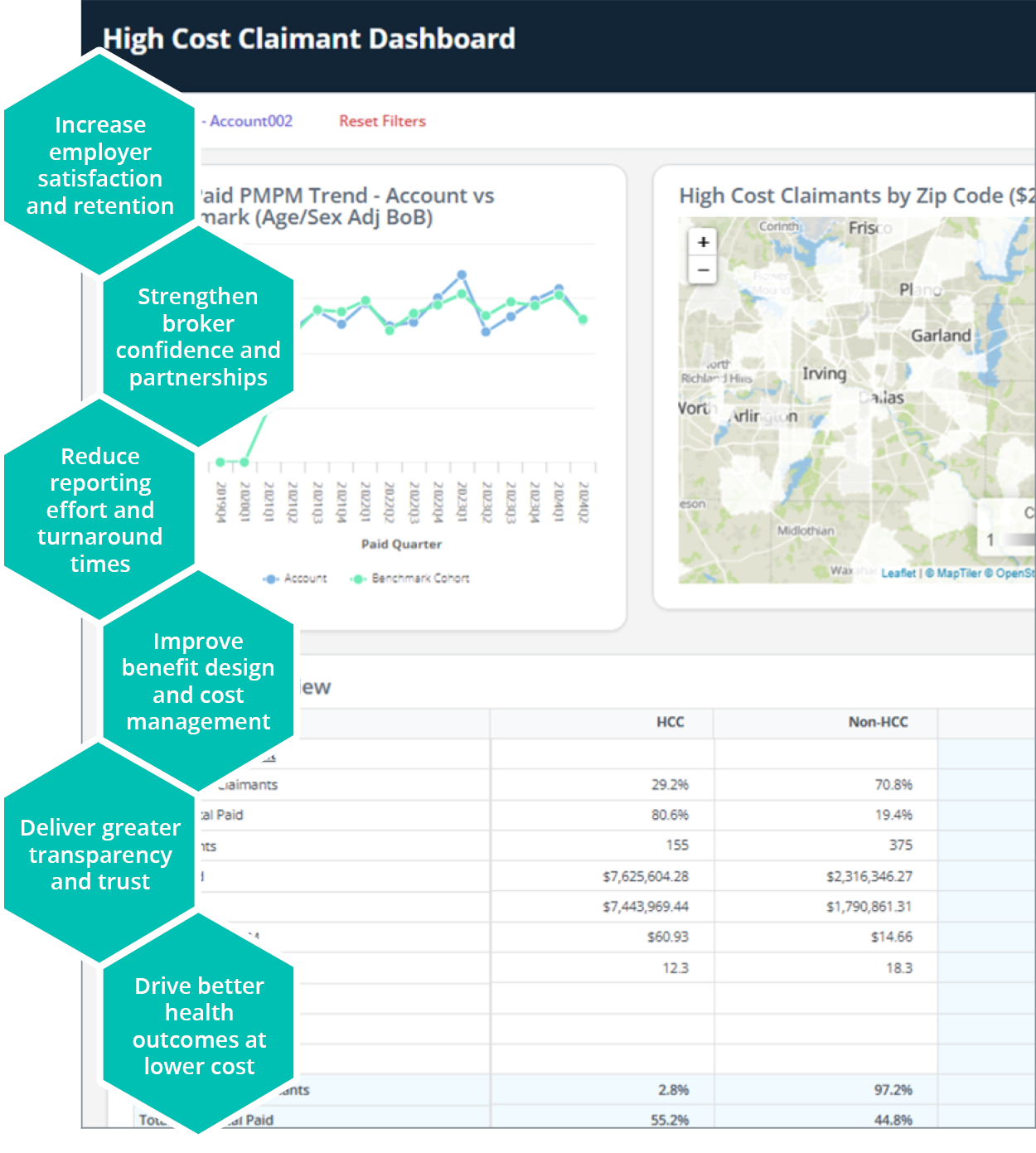
How MedeAnalytics drives value for health plans and their customers.
MedeAnalytics transforms employer reporting into a strategic differentiator to help you:
- Analyze cost, utilization, and trends across groups and sub-groups
- Identify high-cost claimants early and manage stop-loss risk exposure
- Forecast future cost and utilization using predictive analytics
- Benchmark performance against dynamic, relevant datasets
- Integrate social risk insights to better target populations for cost and quality improvements
- Enable interactive reporting and real-time reporting with self-service, customizable views
- Pinpoint and prioritize high utilizers using risk stratification and models and cohort analysis
- Connect insights to action with closed-loop planning, accountability, and measurable results via MedeAchieve
Modernize your employer reporting to strengthen retention, transparency, and growth.
Deliver the insights, transparency, and experience your employer groups expect while positioning your organization for long-term growth. With MedeAnalytics, health plans can provide actionable intelligence and intuitive, employer-friendly experiences that strengthen client retention, reduce reporting burden, optimize benefits, and demonstrate measurable value in every employer relationship.
Learn more about how your analytics can drive action
Excel in customer care while improving staff morale and productivity
After adopting MedeAnalytics Employer Reporting, a northeast health plan achieved record metrics. MedeAnalytics and the health plan collaborated closely to set actionable goals and guiding strategies for successfully deploying the Employer Reporting solution. This in-depth, unified planning effort paid off remarkably. Learn more
Improve client retention and satisfaction with value-added reporting and insights
Health plans must remain competitive in an aggressive market. To do this, plans must show their value by offering their employer and broker clients access to data insights and partner with them to ensure the quality and cost-efficiency of member care. MedeAnalytics Employer Insights provides health plans and their employer group and broker clients with actionable insight into drivers of care cost and quality. Learn more
Monitor and manage he financial impacts of high-cost claimants
As medical and pharmacy costs continue to rise, employers are starting to purchase stop loss policies to help limit these expenses and mitigate against the risk of catastrophic or unpredictable losses. To understand how they are trending against their stop loss policies and predict and understand changes to costs in future policy years, employers require access to clear, comprehensive, and actionable data. Learn more




