Population and Social Risk
Not using integrated social risk data leads to higher costs and lower quality outcomes across all lines of business

80%
of health outcomes are influenced by factors outside of the clinical setting. (Source: American Medical Association)
Fragmented population health and social risk data limit quality outcomes and drive higher costs
Population health strategies often rely primarily on clinical and claims data, leaving out critical social and behavioral factors that drive higher quality outcomes and lower cost.
With data fragmented across systems, organizations lack a complete view of risk, making it difficult to identify high-risk populations, align interventions, and measure impact.
The result is reactive decision-making, misaligned programs, and missed opportunities to reduce utilization, improve outcomes, and control total cost of care.
“We didn’t expect to see everything so quickly. This rapid turnaround was crucial for us as a new plan. Without historical data to rely on, having immediate insights allowed us to understand our performance and chart the path forward. The value we gained from this was immense.”
- Medicare Advantage Plan Executive
MedeAnalytics improves population health and social risk outcomes
See the full picture of risk to deliver true whole-person care.
With MedeAnalytics, you can move from siloed analytics to a unified, intelligence-driven approach to population health and risk management, enabling you to:
- Identify and stratify populations using combined clinical, claims, and social risk insights
- Quantify how risk drivers impact utilization, quality, and total cost of care
- Predict high-cost and high-risk scenarios earlier
- Target interventions with higher precision at both population and individual levels
- Enable more impactful coordinated care and community-based partnerships
- Track outcomes, performance, and ROI across contracts and lines of business
- Improve quality, equity, and Medical Loss Ratio (MLR)
Instead of reactive, retrospective analysis, you gain a proactive, scalable strategy for managing risk and improving outcomes across your populations.

Powered by its enterprise performance platform, MedeAnalytics provides a comprehensive, actuarially grounded view of risk to help organizations move from insight to action at scale.
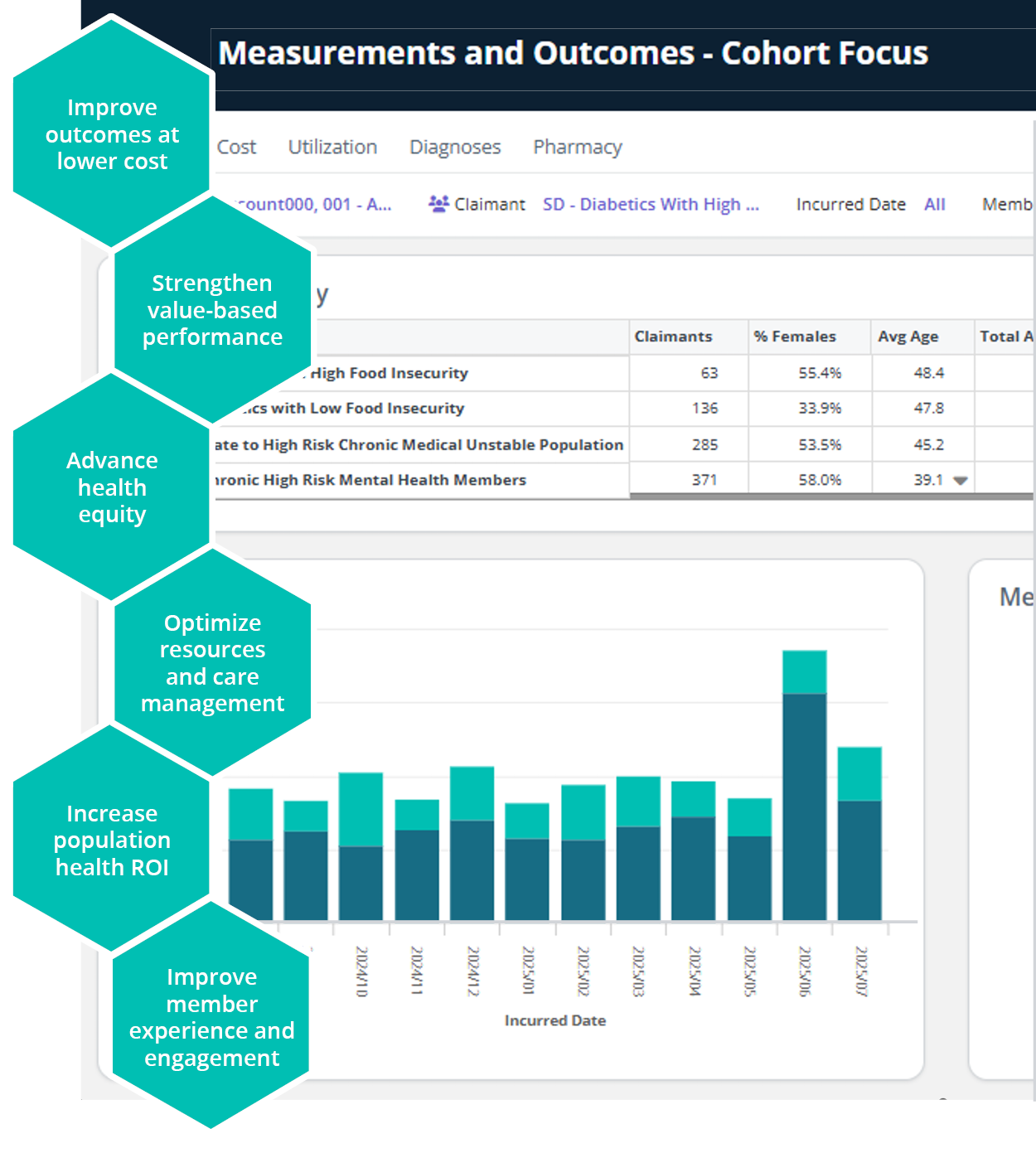
Unlocking strategic value across your population and risk management initiatives
With MedeAnalytics, you can build a scalable, future-ready population health strategy that allows you to:
- Integrate clinical, claims, enrollment, financial, and social risk data into a unified source of truth
- Analyze risk and performance across populations, communities, cohorts, and individuals
- Identify and prioritize high-risk populations using advanced predictive models and risk stratification
- Connect social and clinical factors to utilization, outcomes, and total cost of care
- Enable targeted interventions through precision outreach and care management workflows
- Align with community-based organizations using data-driven collaboration
- Predict program impact before investment and track performance and ROI over time
Elevate your population risk strategy for measurable cost and outcome impact
Transform population health and social risk management into a unified, operational capability. By integrating advanced analytics with real-world data and workflows, you can proactively manage risk, improve care outcomes, advance health equity, and reduce total cost of care across every population you serve.
Learn more about how your analytics can drive action
eBook
How integrated social risk data uncovers millions in hidden value
hile social determinants of health are widely recognized as major cost drivers, most payers lack the integrated analytics infrastructure to identify social risk, quantify its financial effect, and demonstrate ROI on social risk interventions This ebook shares a scalable, enterprise-ready framework for identifying and quantifying the financial impacts of social risk interventions before dollars are spent. Learn more
Case Study
A Southeast health plan achieved up to $25M in validated cost savings
A recent opportunity assessment evaluated the financial impact of integrating social risk into payer analytics. Independent actuarial analysis quantified and validated the significant opportunity social risk presents in driving material cost variation. The health plan client leveraged MedeAnalytics’ Social Risk Insights Measures & Outcomes solution to deliver a comprehensive infrastructure to identify, stratify, intervene, and demonstrate the value of social risk programs. Learn more
Product Overview
Drive improved care quality and outcomes for your members
With today’s heightened focus on care quality, equity, affordability and member satisfaction, health plans are seeking visibility into plan and network performance to improve member care and outcomes. MedeAnalytics' Quality Insights helps payers assess member risk and utilization
and quality of care opportunities through HEDIS® and other quality standards. Learn more



