Quality Performance
Improve HEDIS and Star ratings, close care gaps, and drive better outcomes
Why payers are struggling to improve quality performance.
Payers need timely insights to identify and close care gaps, reduce risk, and improve member experience and outcomes.
Payers are under increasing pressure to improve HEDIS scores, Star ratings, and risk adjustment accuracy while also reducing total cost of care, but quality data is often siloed, delayed, and difficult to act on. As value-based care accelerates, the stakes are even higher. Quality performance now directly impacts reimbursement, member experience, and competitive positioning, making proactive, data-driven improvement essential.
“With MedeAnalytics, we can finally see where our risk truly lies and take action before it impacts our patients or our performance.”
Vice President of Quality, National Health Plan
How MedeAnalytics helps you improve quality ratings and outcomes.
With MedeAnalytics, you can identify care gaps, prioritize interventions, and drive measurable improvements in HEDIS and Star Ratings.
Using advanced healthcare quality analytics and actionable insights, you can track care gaps in real time, stratify members by risk and opportunity, and empower providers and care teams to take the right actions at the right time.

When analytics aren’t actionable, quality leaders, clinicians, and payers face the same challenge—too much data, not enough clarity.
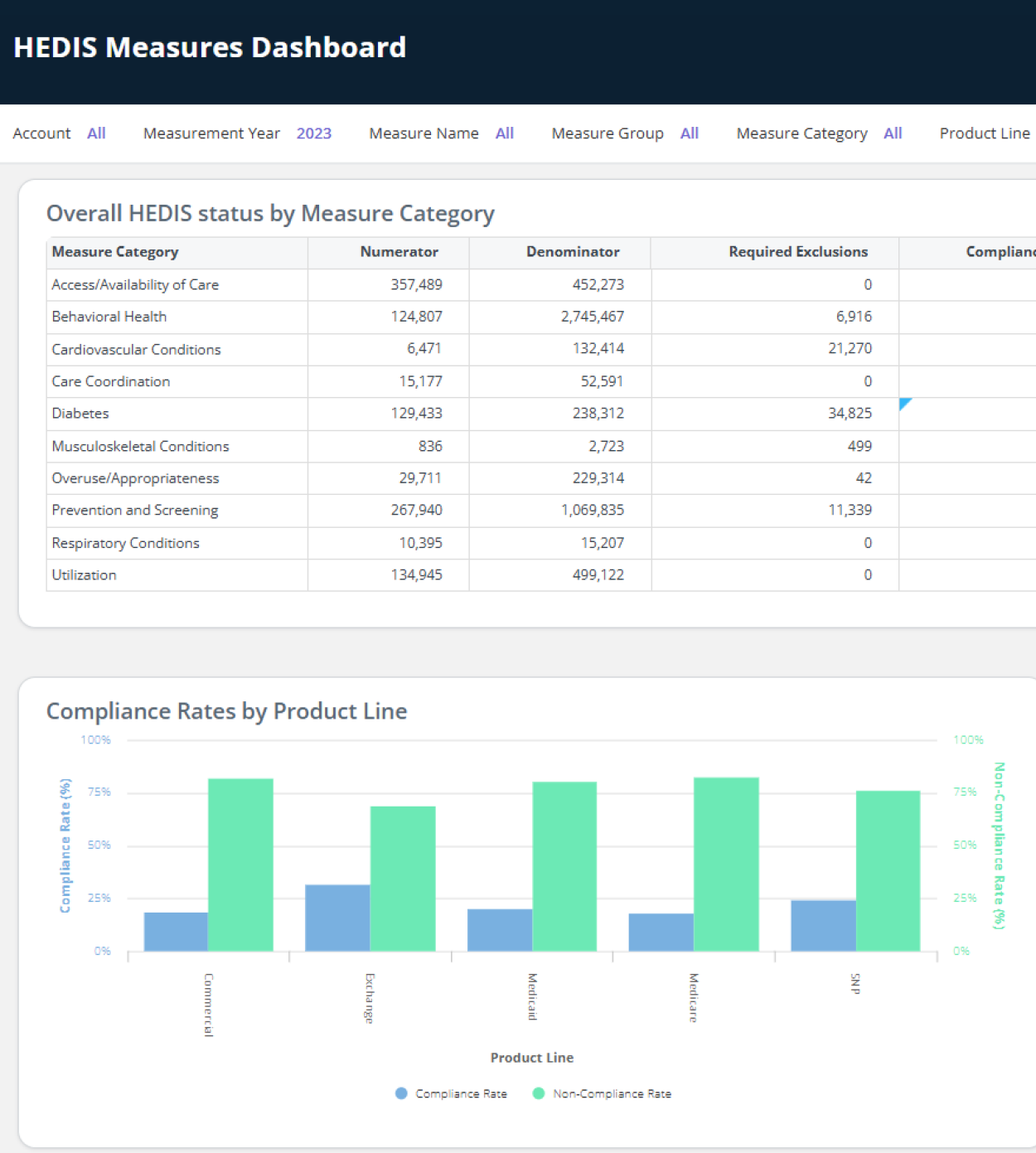
Key capabilities of MedeAnalytics quality performance solutions.
Turn quality improvement into a continuous, data-driven outcomes-focused process with an AI-powered platform that enables you to:
- Track and benchmark HEDIS, AHRQ, hospital-acquired conditions, mortality, and readmission metrics to support proactive quality improvement
- Optimize quality, risk, and financial outcomes to support value-based care and sustainable performance
- Identify high-risk members and patients, predict emerging risks, and enable early intervention
- Stratify risk populations using Adjusted Clinical Groups, Episode Treatment Groups, and Hierarchical Condition Categories
- Streamline risk adjustment and quality reporting across payers and providers to align incentives and drive reimbursement and performance
Elevate your quality performance to improve outcomes, experience, and financial results.
MedeAnalytics combines advanced analytics, expert guidance, and scalable workflows to help payers close care gaps, improve ratings, and deliver better outcomes.
Learn more about how your analytics can drive action
From good to great: Steps to improve your Medicare Advantage Star Ratings
Star Ratings play a crucial role in determining the success and reputation of Medicare Advantage (MA) plans in today’s competitive marketplace. These ratings, often derived from customer feedback and quality metrics, influence consumer choices, regulatory compliance, and financial performance. Learn more
The transition from CMS-HCC V24 to V28: Impacts and strategic steps
The Centers for Medicare & Medicaid Services (CMS) recently announced a significant transition in its risk adjustment model, moving from Version 24 (V24) to Version 28 (V28). Effective January 1, 2024, this change will impact Medicare Advantage (MA) plans, accountable care organizations (ACOs), and other populations within the healthcare system. Learn more
Drive improved care quality and outcomes for your members
With today’s heightened focus on care quality, equity, affordability, and member satisfaction, health plans are seeking visibility into plan and network performance to improve member care and outcomes. MedeAnalytics Quality Insights helps payers assess member risk, utilization,
and quality-of-care opportunities through HEDIS and other quality standards. Learn more




